
Thyroid-Stimulating Hormone (TSH)
At Ultimate Functional Medicine, we believe healing isn’t about chasing symptoms—it’s about creating deep, lasting transformation. These are the three pillars that guide everything we do.
Thyroid-Stimulating Hormone (TSH)
The thyroid plays a critical role in regulating nearly every system in the body—from metabolism and body temperature to energy production and brain function. One of the most commonly measured markers of thyroid health is Thyroid-Stimulating Hormone (TSH).
If you’ve ever had bloodwork done to evaluate thyroid function, chances are your healthcare provider looked at your TSH level first. But what exactly does this hormone do, and what can it tell us about your health?
In this article, we’ll explore what TSH is, why it’s tested, what abnormal levels may indicate, and why looking at the entire thyroid picture is essential for understanding metabolic and endocrine health.
What Is Thyroid-Stimulating Hormone (TSH)?
Thyroid-Stimulating Hormone (TSH) is produced by the anterior pituitary gland, a small but powerful gland located at the base of the brain. The pituitary works closely with the hypothalamus to regulate hormone signaling throughout the body.
Here’s how the thyroid signaling pathway works:
The hypothalamus releases a hormone called thyrotropin-releasing hormone (TRH).
TRH signals the pituitary gland to produce TSH.
TSH then travels through the bloodstream to the thyroid gland, located in the neck.
The thyroid responds by producing two key hormones:
Thyroxine (T4)
Triiodothyronine (T3)
These thyroid hormones regulate:
Metabolic rate
Body temperature regulation
Cardiovascular function
Digestive motility
Lipid and cholesterol metabolism
Brain and neurological function
Energy production at the cellular level
Because thyroid hormones influence so many systems, even subtle imbalances can lead to noticeable symptoms.
How the TSH Feedback Loop Works
TSH operates within a negative feedback loop designed to keep thyroid hormone levels balanced.
When thyroid hormones drop:
The pituitary releases more TSH to stimulate the thyroid gland.
When thyroid hormones rise:
The pituitary releases less TSH, reducing stimulation of the thyroid.
This regulatory system helps maintain stable thyroid hormone levels in the body.
Because of this feedback mechanism, TSH is often used as the first-line screening marker for thyroid dysfunction.
Why Doctors Test TSH
Testing TSH helps clinicians evaluate the thyroid axis, which includes the hypothalamus, pituitary gland, and thyroid gland.
A TSH test is commonly ordered when someone experiences symptoms related to metabolic or hormonal imbalance, including:
Chronic fatigue or low energy
Unexplained weight gain
Difficulty losing weight
Cold intolerance
Low body temperature
Hair thinning or hair loss
Dry skin or brittle nails
Constipation or sluggish digestion
Anxiety or heart palpitations
Heat intolerance
Menstrual irregularities
Fertility challenges
Depression or mood swings
Brain fog or cognitive slowing
Because thyroid hormones regulate metabolism and energy production, even mild dysfunction can significantly impact daily life.
Understanding High TSH Levels
When TSH levels rise above the typical reference range—usually around 4.5–5.0 mIU/L—it often suggests that the thyroid gland is not producing enough hormone.
This condition is known as hypothyroidism.
Common causes of elevated TSH include:
Hashimoto’s thyroiditis (autoimmune thyroid disease)
Iodine deficiency or imbalance
Thyroid removal surgery (thyroidectomy)
Inadequate thyroid hormone replacement therapy
Chronic inflammation or immune dysfunction
When TSH is elevated, the pituitary is essentially sending a stronger signal to the thyroid to increase hormone production.
Symptoms of High TSH / Hypothyroidism
Individuals with elevated TSH often experience symptoms such as:
Persistent fatigue
Weight gain
Cold sensitivity
Constipation
Depression or low mood
Dry skin and hair
Brain fog
Slow metabolism
Reduced exercise tolerance
Even mild elevations—often called subclinical hypothyroidism—may have metabolic consequences depending on the individual and their overall health context.

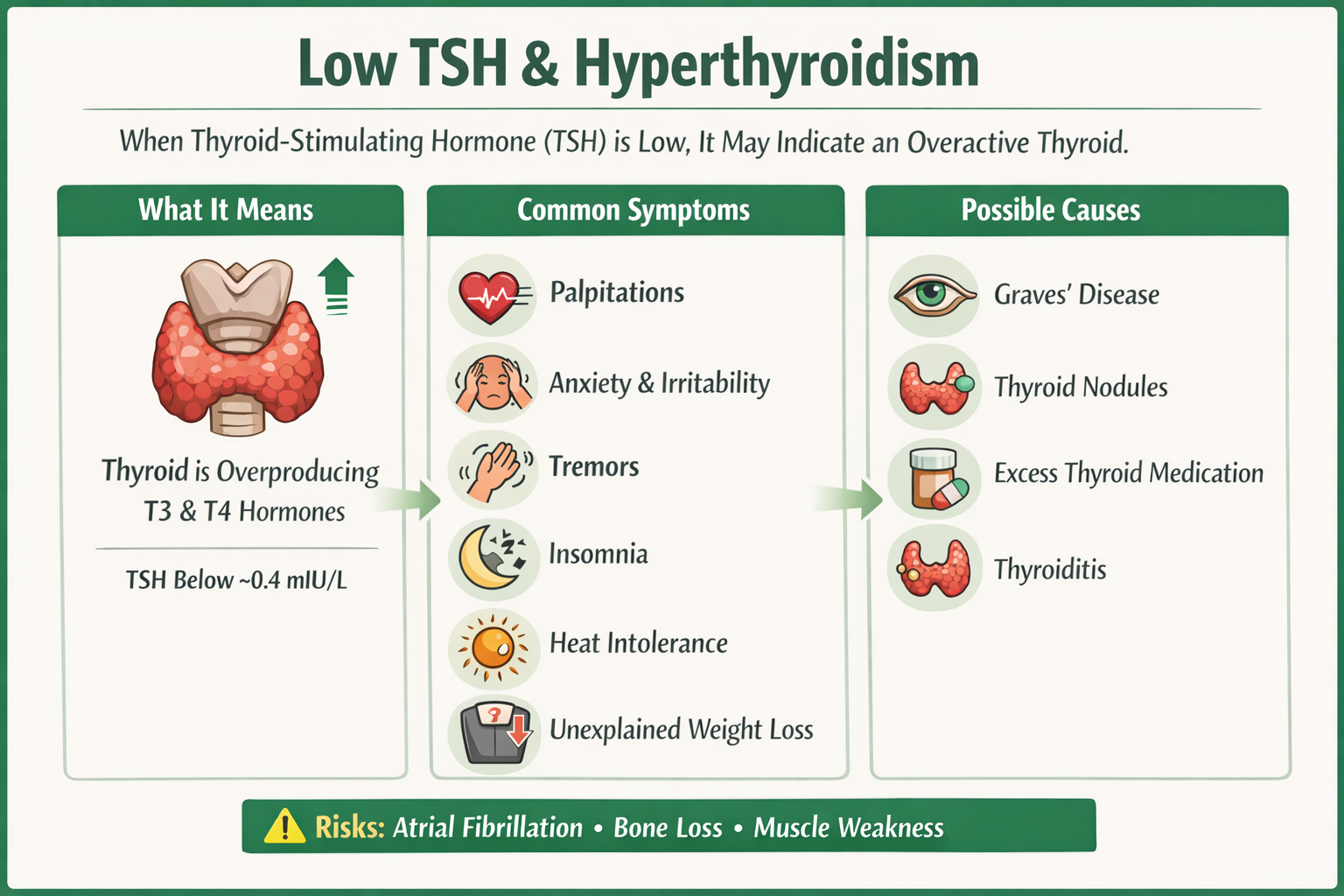
Understanding Low TSH Levels
When TSH levels fall below approximately 0.4 mIU/L, it often indicates hyperthyroidism, a condition where the thyroid produces too much hormone.
Low TSH may occur due to:
Graves’ disease (autoimmune hyperthyroidism)
Thyroid nodules that produce excess hormone
Excess thyroid hormone replacement medication
Transient thyroid inflammation (thyroiditis)
When thyroid hormone levels are high, the pituitary suppresses TSH production to reduce stimulation of the thyroid.
Symptoms of Low TSH / Hyperthyroidism
Low TSH levels can be associated with symptoms such as:
Heart palpitations
Anxiety or nervousness
Tremors
Insomnia
Heat intolerance
Frequent bowel movements
Unintended weight loss
Increased sweating
If TSH remains suppressed for long periods, it may increase the risk of:
Atrial fibrillation
Bone loss or osteoporosis
This is why monitoring thyroid function regularly is important when abnormalities are detected.
Why TSH Alone Isn’t the Whole Story
While TSH is an important marker, it does not directly measure active thyroid hormone levels inside tissues.
In functional medicine and advanced thyroid evaluation, TSH is best interpreted alongside other markers, including:
Free T4 – circulating thyroid hormone available for conversion
Free T3 – the active thyroid hormone that drives metabolism
Reverse T3 – an inactive form that can block thyroid receptors
Thyroid antibodies – markers of autoimmune thyroid disease
Some individuals may have a “normal” TSH but still experience thyroid-related symptoms due to issues such as:
Poor conversion of T4 to T3
Chronic stress affecting hormone signaling
Inflammation or infection
Nutrient deficiencies
Altered thyroid binding proteins
For this reason, TSH should always be interpreted within the broader clinical context, including symptoms and additional lab markers.
Nutrient Factors That Influence Thyroid Function
Several nutrients play a key role in supporting healthy thyroid hormone production and conversion.
Important thyroid-supportive nutrients include:
Iodine – essential for thyroid hormone production
Selenium – supports T4-to-T3 conversion
Iron – required for thyroid enzyme activity
Zinc – supports thyroid receptor sensitivity
Tyrosine – amino acid building block of thyroid hormones
Deficiencies in these nutrients may contribute to thyroid imbalance even when TSH appears normal.

The Importance of Monitoring Trends
A single TSH measurement provides a snapshot of thyroid signaling at one moment in time. However, tracking TSH trends over months or years often reveals more meaningful insights.
Gradual increases or decreases may indicate:
Emerging thyroid dysfunction
Stress-related hormone shifts
Changes in medication needs
Nutrient deficiencies
Monitoring trends helps clinicians identify patterns and intervene earlier when necessary.
Final Thoughts
Thyroid-Stimulating Hormone (TSH) is a powerful marker that reflects how the brain communicates with the thyroid gland to regulate metabolism and energy production.
However, TSH should never be interpreted in isolation. Understanding thyroid health requires a broader view that includes hormone levels, nutrient status, immune activity, and clinical symptoms.
If you are experiencing symptoms such as fatigue, weight changes, mood fluctuations, or temperature sensitivity, a comprehensive thyroid evaluation may provide valuable insight into your overall metabolic health.
Working with a knowledgeable healthcare provider can help uncover the root causes of thyroid imbalance and create a personalized plan to restore optimal function.
Join a New Model of Medicine
We created Ultimate Functional Medicine because we believe you deserve more than symptom suppression.
You deserve answers.
You deserve clarity.
You deserve a care team that treats you like a whole person—not just a case file.
If you’re tired of feeling dismissed or stuck...
If you’re ready to get to the root of what’s going on...
If you want a personalized, empowering path to healing...
Then we invite you to step into this new model of medicine with us.
This isn’t alternative. It’s advanced.
It’s not fringe—it’s foundational.
And it just might be the approach you’ve been looking for all along.
📞 Ready to get started?
Book your Root Cause Discovery Call and let’s explore how these three pillars can support your healing journey.
